How PT Helps Avoid Injuries
- By Todd Aalbu, MPT, CSCS, PES, CAFS
- •
- 30 Mar, 2016
- •
Maintaining Core Strength Key

I have finally decided to take the plunge and add a blog to my site. I always wanted an easy way to share information with visitors and I’m super excited to start this journey. Keep coming back to my site and check for updates right here on the blog.

So, I start this entry at the finale of week 4 post-op, which concluded with a successful week in Physical Therapy where goals were met, and the 1-month post-op visit with Brad, Dr. Khalfayan’s PA.
I titled this entry as “Reality Bites” due to the fact that, again, unrealistic expectations often will lead to disappointment. I had the thought earlier this week that the definition of “Reality” should be “where Theory converges with Execution/Performance.” You might have the unrealistic expectation that you are going to be ahead of the average, but then the physical fact that healing occurs at a fairly set rate, and regardless of who you think you will be, there are only so many factors that can influence that rate of healing.
I have come to the realization that this is, in-fact, a very long road to recovery. Theory and knowledge of the healing process and Rotator Cuff function would have clearly defined that fact. But when you go into the procedure with unrealistic expectations of beating the “protocol,” it set me up for being unprepared for some of the typical ups and downs that occur with recovery.
So, my PT, David Dahl, has had the unfortunate task of having to “talk me off of the ledge” a couple of times this week. Bringing things back into perspective that we have met the goals of the protocol, as well as that this is only week 4 after surgery, of what Dr. Khalfayan has predicted to be a 10-12 month recovery to full function. With that perspective, I have to keep in mind that this is roughly 1/12 of the way in the process. Brad at my 4-week post-op visit drove this point home as well, stating that being at this point in the recovery process is exactly where they want to see me, not ahead of schedule, and not behind. In their experience, Brad included that the individuals who are ahead of the protocol and schedule often are more at risk for re-tear/failure of repair. The individuals who are way ahead of schedule often falsely gain confidence and push activities past what the repair can handle to which leads to the failure of the repair.
To re-focus on the positives, I am sleeping in bed propped up. As well as sleeping in bed, I am also now able to make it through a better part of the night sleeping roughly 3 hours at a time, before changing positions, and then going back to sleep. I have also been able to sleep a few hours without my sling on, with is a very welcomed change! I have been driving this week for short distances as well as spending a little time at work doing some light computer work and paper work. All of these seem minor, but feel like exponential gains from 1-2 weeks ago. Progress is occurring!!
I titled this entry as “Reality Bites” due to the fact that, again, unrealistic expectations often will lead to disappointment. I had the thought earlier this week that the definition of “Reality” should be “where Theory converges with Execution/Performance.” You might have the unrealistic expectation that you are going to be ahead of the average, but then the physical fact that healing occurs at a fairly set rate, and regardless of who you think you will be, there are only so many factors that can influence that rate of healing.
I have come to the realization that this is, in-fact, a very long road to recovery. Theory and knowledge of the healing process and Rotator Cuff function would have clearly defined that fact. But when you go into the procedure with unrealistic expectations of beating the “protocol,” it set me up for being unprepared for some of the typical ups and downs that occur with recovery.
So, my PT, David Dahl, has had the unfortunate task of having to “talk me off of the ledge” a couple of times this week. Bringing things back into perspective that we have met the goals of the protocol, as well as that this is only week 4 after surgery, of what Dr. Khalfayan has predicted to be a 10-12 month recovery to full function. With that perspective, I have to keep in mind that this is roughly 1/12 of the way in the process. Brad at my 4-week post-op visit drove this point home as well, stating that being at this point in the recovery process is exactly where they want to see me, not ahead of schedule, and not behind. In their experience, Brad included that the individuals who are ahead of the protocol and schedule often are more at risk for re-tear/failure of repair. The individuals who are way ahead of schedule often falsely gain confidence and push activities past what the repair can handle to which leads to the failure of the repair.
To re-focus on the positives, I am sleeping in bed propped up. As well as sleeping in bed, I am also now able to make it through a better part of the night sleeping roughly 3 hours at a time, before changing positions, and then going back to sleep. I have also been able to sleep a few hours without my sling on, with is a very welcomed change! I have been driving this week for short distances as well as spending a little time at work doing some light computer work and paper work. All of these seem minor, but feel like exponential gains from 1-2 weeks ago. Progress is occurring!!

Not being a person who enjoys being the “center of attention,” I am stepping out of my comfort zone to document my journey through some of the details of my rehabilitation of my right shoulder. It has been a long time in coming, as my injury occurred in January of 2016, in which I had an unfortunate pre-release of my front binding while I was slalom skiing (waterskiing). As I was crossing into the first wake, my front foot literally stepped out of the binding, to which with my forward momentum, I came down into the water leading with my right shoulder. It happened quick enough without warning, and I cannot recall if it was the handle, or just the force of the water, that then threw my right arm up over my head with enough velocity to cause the injury.
At the time, I knew that this injury was “more than the typical fall” that with some time, some rest, and usually some ibuprofen, I would get past the inflammatory phase and move on. Within a few days, as the acute phase was calming down, I was able to understand that I had some hallmark signs of instability of my shoulder, which lead me to seek out an Orthopedic consult with a local Ortho surgeon. A MRI was ordered and results found a tear of my Posterior Labrum, as well as what was thought to be a small tear in my Supraspinatus Muscle/Rotator Cuff. A cortisone injection was administered, with little relief, which lead to another injection approximately 4 weeks later.
One thing that I often will counsel my clients on is that “you often have to be your own medical advocate,” leading you to make decisions or determine the best course of treatment for your own benefit. It is interesting how I can often recognize that need in my own clientele, but that it is so often ignored when YOU are the CLIENT. I say this only because that during the months after my initial injury, my “gut” told me that there was more going on, even though the course of treatment suggested was fairly routine and very conservative. None-the-less, I continued on the conservative trail, trying to manage my symptoms with rest, stretching, and avoiding activities or positions that seemingly were aggravating my inflammation. All the while I was avoiding what was truly staring me in the face, and that was the fact that I was getting weaker, having tremendous difficulty sleeping at night as well as working, limiting my skiing frequency significantly, and growing more and more frustrated with my condition. It was upon seeing the Ortho again one time in May that I expressed my frustration at my lack of progress, to which they said, “Well Todd, you are really just dealing with an inflamed bursitis, nothing more.” I was very perplexed by this statement, as I had a confirmed Rotator Cuff tear, as well as a Labrum tear from the MRI. But, I did not want to be confrontational with the MD, so I walked out of that appointment knowing that I would be needing to seek a second opinion. Finally, I started to wake up and follow my gut instinct. Be that as it may, it only took me 8 months to figure it out…
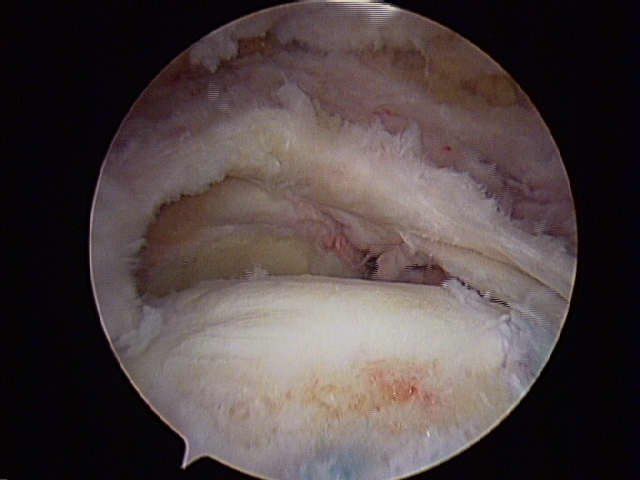
Fast forward to September, and my consult with the second opinion. I chose an Orthopedic Surgeon in Seattle who has a great reputation, and a surgeon that I have seen phenomenal outcomes from their surgical decisions and techniques. He took one look at the MRI, and noticed more involvement that had previously been noted by the first Ortho, as well as the need for further testing involving a contrast dye Arthrogram to indicate the full involvement of the injury. After a few weeks of aggressive PT for what was now an adhered capsule (aka “frozen shoulder”), the Arthrogram was conducted. What was indicated was a 1-inch tear (2.5 cm) in one direction, as well as another roughly 1-inch tear (2.2 cm) in another direction of the Supraspinatus. It also showed not only the tear in the Posterior Labrum, but also a tear of my Anterior Labrum (SLAP), as well as some other “43-year old shoulder” arthritic changes. In the next blog, I will further go into the next step, “To do surgery or continue the conservative route.”
At the time, I knew that this injury was “more than the typical fall” that with some time, some rest, and usually some ibuprofen, I would get past the inflammatory phase and move on. Within a few days, as the acute phase was calming down, I was able to understand that I had some hallmark signs of instability of my shoulder, which lead me to seek out an Orthopedic consult with a local Ortho surgeon. A MRI was ordered and results found a tear of my Posterior Labrum, as well as what was thought to be a small tear in my Supraspinatus Muscle/Rotator Cuff. A cortisone injection was administered, with little relief, which lead to another injection approximately 4 weeks later.
One thing that I often will counsel my clients on is that “you often have to be your own medical advocate,” leading you to make decisions or determine the best course of treatment for your own benefit. It is interesting how I can often recognize that need in my own clientele, but that it is so often ignored when YOU are the CLIENT. I say this only because that during the months after my initial injury, my “gut” told me that there was more going on, even though the course of treatment suggested was fairly routine and very conservative. None-the-less, I continued on the conservative trail, trying to manage my symptoms with rest, stretching, and avoiding activities or positions that seemingly were aggravating my inflammation. All the while I was avoiding what was truly staring me in the face, and that was the fact that I was getting weaker, having tremendous difficulty sleeping at night as well as working, limiting my skiing frequency significantly, and growing more and more frustrated with my condition. It was upon seeing the Ortho again one time in May that I expressed my frustration at my lack of progress, to which they said, “Well Todd, you are really just dealing with an inflamed bursitis, nothing more.” I was very perplexed by this statement, as I had a confirmed Rotator Cuff tear, as well as a Labrum tear from the MRI. But, I did not want to be confrontational with the MD, so I walked out of that appointment knowing that I would be needing to seek a second opinion. Finally, I started to wake up and follow my gut instinct. Be that as it may, it only took me 8 months to figure it out…
Fast forward to September, and my consult with the second opinion. I chose an Orthopedic Surgeon in Seattle who has a great reputation, and a surgeon that I have seen phenomenal outcomes from their surgical decisions and techniques. He took one look at the MRI, and noticed more involvement that had previously been noted by the first Ortho, as well as the need for further testing involving a contrast dye Arthrogram to indicate the full involvement of the injury. After a few weeks of aggressive PT for what was now an adhered capsule (aka “frozen shoulder”), the Arthrogram was conducted. What was indicated was a 1-inch tear (2.5 cm) in one direction, as well as another roughly 1-inch tear (2.2 cm) in another direction of the Supraspinatus. It also showed not only the tear in the Posterior Labrum, but also a tear of my Anterior Labrum (SLAP), as well as some other “43-year old shoulder” arthritic changes. In the next blog, I will further go into the next step, “To do surgery or continue the conservative route.”